.png)

99%
Reduction in denials
$0
Claim backlog
3x
ROI on your billing staff
Meet the Operating System
Your team feels like they can’t catch up.
Billing that is not built for behavioral health costs you in hours to verify benefits, scrub claims, and address denials.


Step 01
Verify Insurance for Behavioral Health
Eric checks eligibility in real time before every appointment — catching coverage gaps, inactive plans, and behavioral health carve-outs before they become denied claims.
- Real-time payer eligibility checks across all major insurers
- Behavioral health benefit verification including carve-outs
- Flags issues before the appointment, not after billing
- Automatic re-verification for recurring patients
Step 02
Review & Submit
Clean Claims
Clean Claims
Eric reviews every claim in the queue, scrubs for errors, and submits — continuously. No more backlogs, no more delayed collections.
- Automated claim scrubbing before every submission
- Works the queue continuously — claims never pile up
- Claims scrubbed with your custom contract rules and behavioral health best practices
- Submission confirmations tracked in real time
.png)
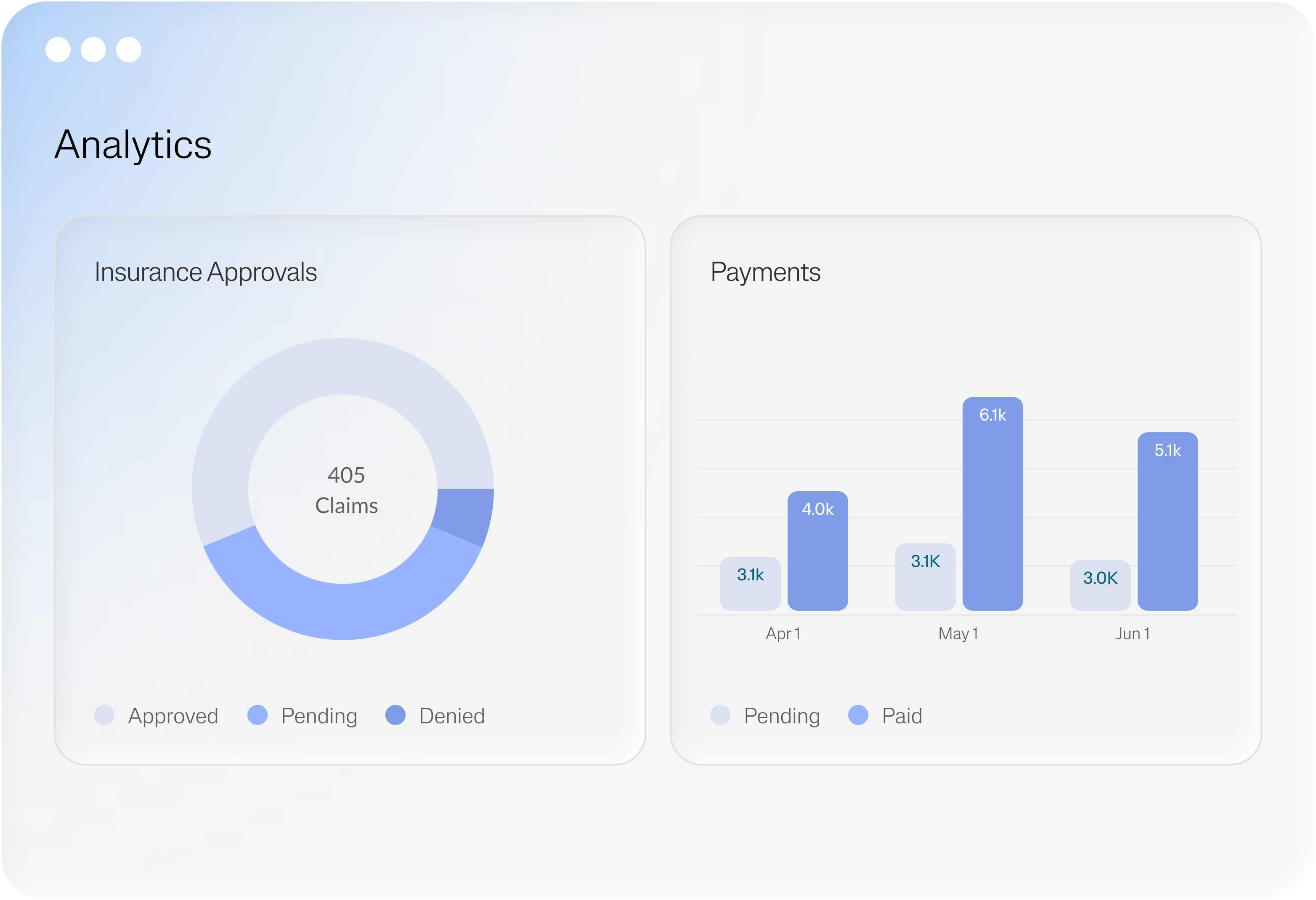
Step 03
Monitor Denials &
Payer Behavior
Payer Behavior
Eric doesn't just react to denials — it learns from them. Every resolved denial makes the system smarter, shifting your team from firefighting to strategy.
- Real-time denial tracking across all payers
- Pattern detection — spots payer-specific denial trends
- Automated appeal preparation and resubmission
- System gets smarter with every resolved denial
Capabilities
Everything
Eric handles.
Insurance Verification
Catch eligibility issues before they become denied claims. Real-time checks for every patient, every visit.
Clean
Claims
Claims
Submit right the first time, every time. Eric scrubs every claim before it goes out.
Payer Intelligence
Learn payer behavior and get smarter with every denial. Strategic improvement built in.
Zero
Backlog
Backlog
Eric works the claim queue continuously, so claims never pile up and collections never slow down.












